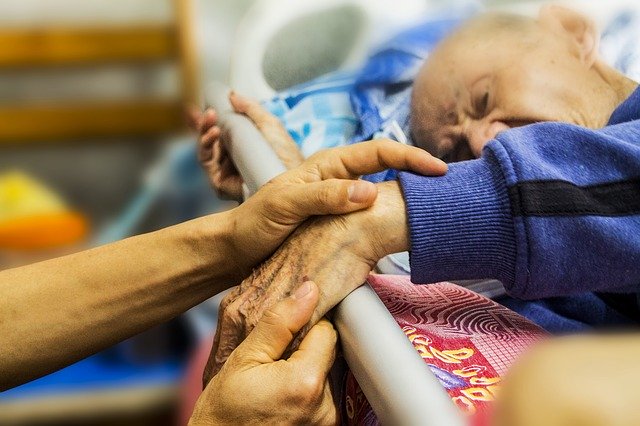
One of the most uncomfortable and risky signs of nursing home negligence is the appearance of bedsores.
The human body is meant to be mobile and works best when it is challenged (within reason). When an elderly person is left alone and not moved from a prone to a sitting position damages begins to accumulate. The skin can tear, and continuous pressure leads to injury.
Even for patients with low mobility, it is important to reposition the body to even out pressure and let the skin breath a bit.
Causes
Start with learning that bedsores, also called pressure ulcers or decubitus ulcers, form in areas where heat and pressure are higher.
Add in a little friction and subdermal tissue can tear. The tear allows in blood, and after infection, pus. These increase the pressure, widening the tear and causing discomfort. The pain leaves a person leaning away from the area of the pain, which increases pressure on other areas which can then develop further sores.
Sores develop in the sensitive skin areas and areas that deal with the largest amount of weight. Areas in the tailbone and hips, and the groin region are common and exceptionally painful.
Other risk areas include the heels, ankles, and upper thighs or arms. Any area that frequently pushes into a bed or chair and doesn’t get enough time to breathe or cool down between states.
Any overly sedentary position or behavior can increase the risks of bedsores and prolong the condition once it starts. Movement after a bedsore has started tends to rupture the tissue and cause drainage, which can spread the risk of secondary infection.
Prevention is Paramount
The problem with bed sores is that they tend to get worse once they form as they need time to heal and time also is one of their leading causes.
The best way to deal with bedsores, then, is to prevent them in the first place.
An active lifestyle and adequate but not prolonged rest are key to preventing issues. The elderly are at an enhanced risk of bedsores, not just from additional rest and sitting but because the skin loses elasticity as collage a depletes. This makes it easier for tears to form.
A rich diet keeps skin healthy longer. Routine bathing and hygiene rejuvenate skin and keeps moisture levels in check.
All of these preventative measures are built-in to a vigorous lifestyle and fall under routine maintenance care at a facility. When care levels decline, it’s easy to see how bedsores can quickly become present.
Risk Factors
Bedsores create pain and can rupture, which both leaves a site open for infection and a can spread infection.
The pain leads to decrease mobility, which feeds into the cycle. The sores also tend to unsightly and can cause social stress as well. Advanced bedsores may have a smell associate which further isolates a sufferer.
It’s been shown that such psychological stresses leach vital peptides from skin, necessary for elasticity and building of tissue. In this way, one bed sore can also lead to more by reducing overall skin health from the net stress.
Stay Vigilant
It’s hard to see your loved ones suffer. Getting older carries with it increased risk for so many different aliments and struggles. It’s important that those providing care do an exemplary job to keep elders happy and healthy.
When this quality of care breaks down, it’s important to intervene. If you suspect nursing home negligence is affecting your loved ones, contact us to learn what to do next. We’re here to help.